-
-
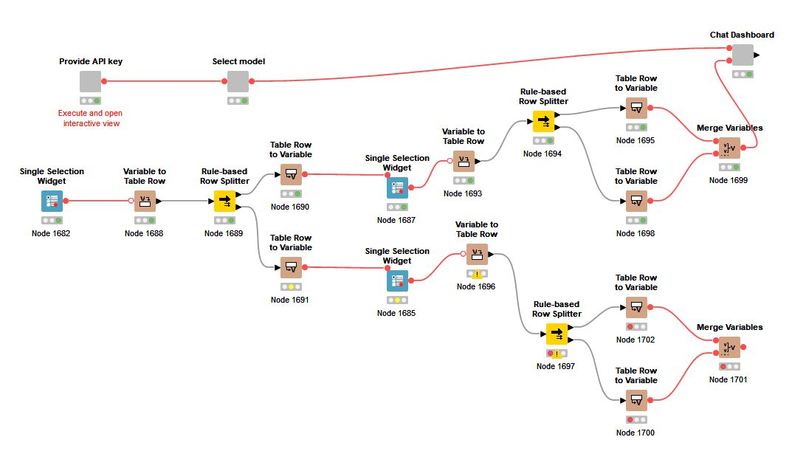
Fig 1: The Knime workflow visualization.
-
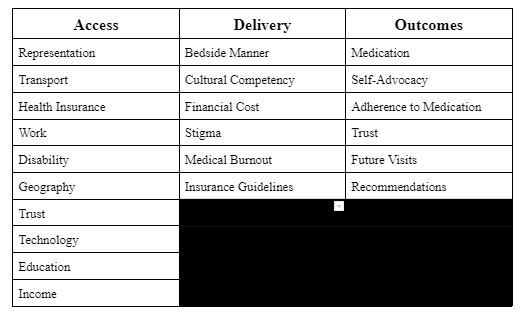
Fig 2: Areas for Potential Gaps in Equity and Diversity in Healthcare.
-
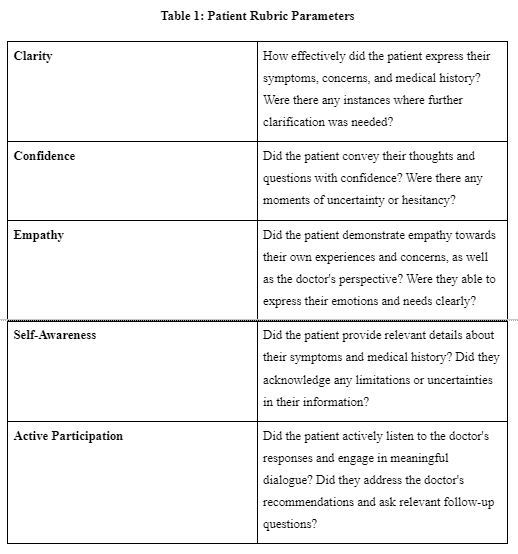
Table 1: Patient Rubric Parameters
-
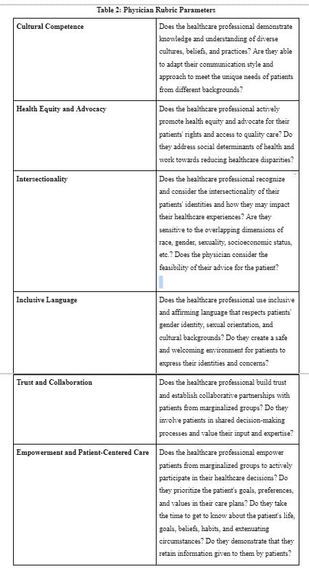
Table 2: Physician Rubric Parameters
-

Fig 3: Rubric result for positive doctor-patient interaction.
-

Fig 4: Rubric result for negative doctor-patient interaction.
-

Fig 5: Example of a physician character prompt.
-

Fig 6: Example of a patient character prompt.
-

Fig 7: The initial prompt instructions for all characters.
-

Fig 8: The rubric instructions, which end the context prompt.
Statement of the Problem
Healthcare is a field that has been long established as one that focuses on building rapport and providing for patients. Its fundamental purpose is to enhance the quality of one’s life by improving one’s health. In order to further the quality and reach of healthcare in society, it is crucial to bear in mind the inherent stigmas and unconscious biases present in both hospital staff and patient populations. Clinical staff, regardless of geopolitical affiliation, carry inherent biases that present barriers to providing high quality care to patients. As stated by Nsiah et al., a lack of patient advocacy has inevitable negative consequences that result in complications of current conditions or death as a direct result of physicians/healthcare workers unwillingness to treat patients in a reasonable amount of time (2019, p.2). This lack of patient advocacy leading to secondary conditions and complications is also reflected in Houlihan’s study in which he claimed that 80% of the problems mentioned by patients with Spinal Cord Injuries (SCI) were related to secondary conditions, such as Urinary Tract Infections (UTIs) (2016). He also stated that more than half of patient contact with primary care providers (PCPs) were related to secondary conditions; a third of which were considered preventable. It was also found that half of all ED visits pertinent to SCIs were considered preventable and/or lower urgency. Furthermore, Houlihan states that 33% of individuals with SCIs have unmet primary care needs, particularly in individuals with lower socioeconomic status (2019). In order to alleviate this burden amongst patient populations, it is crucial to create a data-driven application that is able to identify disparities, promote diversity, and establish equity amongst the field of healthcare. To design such a product, data would need to be collected from various sources, including but not limited to journal articles and anecdotal evidence, from both patients and healthcare workers to ensure both sides of the discussion are accurately represented.
Objective
Our main objective with this project is to create an advanced API integrated with Knime and ChatGPT with predefined grading parameters that is able to test/educate both providers and patients with a training simulation to become more effective communicators to provide higher quality care and increase patient advocacy. The rubric for grading the interaction was created by the team, expanded through ChapGPT, and verified via discussion amongst the team and clinical articles.
Rubric
It was seen that in the United States, members of the African American community are particularly susceptible to these poor interactions as a result of systematic distrust in the American Healthcare System. Unethical clinical trials that targeted the African American community, such as the Tuskegee Syphilis Study (Kennedy, 2007), have had a butterfly effect leading to disparities in all aspects of healthcare. This includes, but is not limited to issues among African American men, women, and children receiving care and often being overlooked, as well as significant mental health disparities among African Americans (Mitchell, 2021)
Parameters for the rubric were created by brainstorming and created an extensive list of the issues that we believed were prevalent in the medical community. This list was divided into 3 main domains: Access, Delivery, and Outcomes. Below each of these 3 domains a large list was compiled, from which a final rubric was created. This allowed us to create a mini-database from which we were able to determine the issues that we could most effectively address with a novel solution while utilizing KNIME. While creating this list, a theme appeared between the Access and Delivery domains: poor communication. Poor communication between healthcare providers and patients alike is a significant impediment to high quality care. This issue is also seen in various studies in which they found that ineffective/poor communication results in 27% of medical malpractice (Tiwary, 2019). This lack of clear and concise communication, both on a macro and micro level, causes speed bumps in what would be a smooth transaction resulting in lack of trust, stigmas regarding treatment, and in a general sense, inadequate knowledge regarding procedures, conditions, and medications.
Solution: Utilize KNIME workflows in conjunction with OpenAI’s GPT-4 model to develop an end-to-end deliverable that can train/teach physicians and patients in clear, compassionate, and culturally competent communication. Thus, the 5C Model. Prompts were written with a set of guidelines to create characters for this solution.
Description of the Deliverable
Our meticulously designed KNIME workflow integrates with the ChatGPT API, empowering users to engage in dynamic conversations with virtual characters. Upon accessing the dashboard, users are prompted to select their role as either a patient or a doctor. This choice unlocks a range of diverse characters, each imbued with their unique backgrounds, beliefs, biases, and attitudes, thereby creating an immersive and authentic learning environment.
Each doctor was designed to have an internal bias that would serve as a barrier to communication with their patients, as well as several quirks as to how they personally practice medicine. This intentional approach encourages patients to cultivate self-advocacy skills as they navigate these interactions, developing strategies to advocate for their needs and overcome potential obstacles. On the patient side, each character exhibits a quirk, which varies from a required disability accommodation to a fear of hospitals. These individual idiosyncrasies compel healthcare providers to carefully consider the patient's perspective, empathize with their concerns, and tailor their approach accordingly. By prompting doctors to think critically about patient experiences, our solution aims to foster a more patient-centered healthcare ecosystem.
Our dashboard incorporates a comprehensive rubric for each scenario, fostering growth and improvement by systematically evaluating user performance across various categories. Tailored to the specific social deficits of doctors and patients, the rubric criteria provide targeted assessments to enhance healthcare practices. For doctors, the rubric assesses cultural competence, health equity and advocacy, intersectionality, inclusive language, trust and collaboration, and empowerment and patient-centered care, offering invaluable insights and actionable feedback to deliver more equitable healthcare services. For patients, the rubric evaluates clarity, confidence, empathy, self-awareness, and active participation, providing a structured framework for self-reflection and empowering patients to cultivate self-advocacy skills and assert their voice in healthcare decision-making processes.
Conclusion
In a world where effective communication and equitable healthcare are fundamental pillars of well-being, the integration of KNIME workflows and the transformative power of ChatGPT offer an extraordinary opportunity for change. Our innovative solution, powered by the synergy of advanced technology and human-centered design, has the potential to revolutionize the future of medicine. By immersing users in dynamic conversations with diverse virtual characters, our dashboard creates a rich learning environment that transcends traditional training methods. Doctors and patients alike are challenged to navigate the complexities of bias, quirks, and unique perspectives, fostering empathy, understanding, and self-advocacy. Through the lens of our comprehensive rubric, we empower healthcare providers to evaluate and enhance their cultural competence, promote health equity, consider intersectionality, employ inclusive language, build trust and collaboration, and prioritize patient-centered care. At the same time, patients are encouraged to express themselves with an element of clarity and confidence. In addition, we hope that it will allow patients to embrace empathy, deepen their own self awareness, and become active participants in managing their care.
We envision a future where healthcare is free from barriers of stigma and bias, and our solution paves the way for a more inclusive, conscientious, and patient-centered healthcare ecosystem. The impact from such a product is profound; creating a world of healthcare where every voice is heard, every perspective valued, and every patient’s needs met. Imagine a world where doctors are not only skilled practitioners but also compassionate advocates, and patients are empowered to navigate their healthcare journeys with confidence and clarity. This is the future that our ChatGPT-powered dashboard holds the promise of creating. As we conclude the weekend, we invite the judges to join us in embracing the limitless potential of these technologies. Let us envision and work towards a future where diversity and equity are not just ideals, but day-to-day practices within the field of medicine, ultimately creating a healthier, more welcoming world.
What we learned
During the development of our project, we embarked on a journey of learning and discovery. We successfully integrated KNIME into our platform, harnessing its powerful data analytics and workflow capabilities. Through extensive experimentation, we gained a deep understanding of how to leverage KNIME for data preprocessing, analysis, and visualization.
Developing and testing ChatGPT-powered NPCs was a dynamic and iterative process. We crafted diverse character templates, carefully considering their cultural backgrounds, communication styles, biases, and quirks. Through multiple iterations and feedback loops, we refined the NPCs to create more realistic and immersive interactions.
Throughout the development journey, we learned the importance of continuous improvement and adaptation. We actively sought user feedback and made iterative updates based on their experiences. This iterative approach allowed us to fine-tune the system, enhancing its accuracy, cultural sensitivity, and overall user experience.
What's next for UnityMed: Advancing Cultural Sensitivity in Healthcare
Moving forward, our next steps involve further enhancing the capabilities of our KNIME workflow to administer and store rubric scores, enabling us to track progress in scoring over multiple interactions. This will provide valuable insights into the effectiveness of our system and allow us to make data-driven improvements.
We recognize the importance of refining the prompts to incorporate more character nuance. Our aim is to create a more authentic and immersive experience by enabling the NPCs to speak in cultural vernacular or express emotions such as anger when provoked. Consistency in character expression across all prompts and characters will be a key focus, ensuring that the NPCs respond in a cohesive and believable manner. To achieve this, we will curate diverse prompts, incorporating cultural references and emotional responses. User feedback will be instrumental in fine-tuning the system and ensuring authenticity.
By combining the power of KNIME's workflow management and data analytics with our commitment to developing culturally nuanced prompts, we aim to create a robust and dynamic system that delivers immersive, personalized, and culturally inclusive experiences for our users.
References
Houlihan, B., Brody, M., Plant, A., Skeels, S. E., Zazula, J., Pernigotti, D., Green, C., Hasiotis, S., & Jette, A. (2016). Health care self-advocacy strategies for negotiating health care environments: Analysis of recommendations by satisfied consumers with SCI and SCI practitioners. Topics in Spinal Cord Injury Rehabilitation, 22(1), 13–26. https://doi.org/10.1310/sci2201-13
Kennedy, B. (2007). AFRICAN AMERICANS AND THEIR DISTRUST OF THE HEALTH CARE SYSTEM: HEALTHCARE FOR DIVERSE POPULATIONS. Journal of Cultural Diversity, 14(2), 56–60.
Mitchell RN, A. (2021). African Americans healthcare disparities and inclusive practice; A literature review. Journal of Quality in Health Care & Economics, 4(1). https://doi.org/10.23880/jqhe-16000199
Nsiah, C., Siakwa, M., & Ninnoni, J. P. K. (2019). Registered Nurses’ description of patient advocacy in the clinical setting. Nursing Open, 6(3), 1124–1132. https://doi.org/10.1002/nop2.307
Tiwary, A., Rimal, A., Paudyal, B., Sigdel, K. R., & Basnyat, B. (2019). Poor communication by health care professionals may lead to life-threatening complications: Examples from two case reports. Wellcome Open Research, 4, 7. https://doi.org/10.12688/wellcomeopenres.15042.1
Built With
- chatgpt
- knime










Log in or sign up for Devpost to join the conversation.