-
-
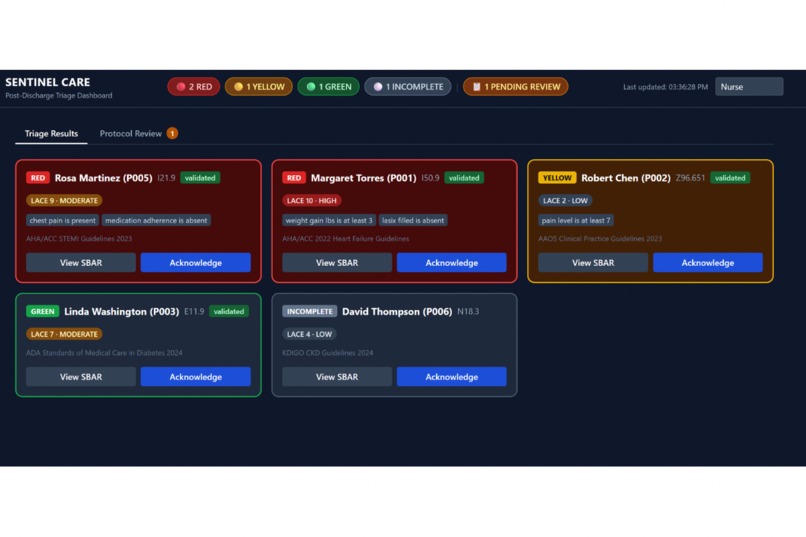
Live triage dashboard with 5 patients sorted by urgency across RED, YELLOW, GREEN, and INCOMPLETE states.
-
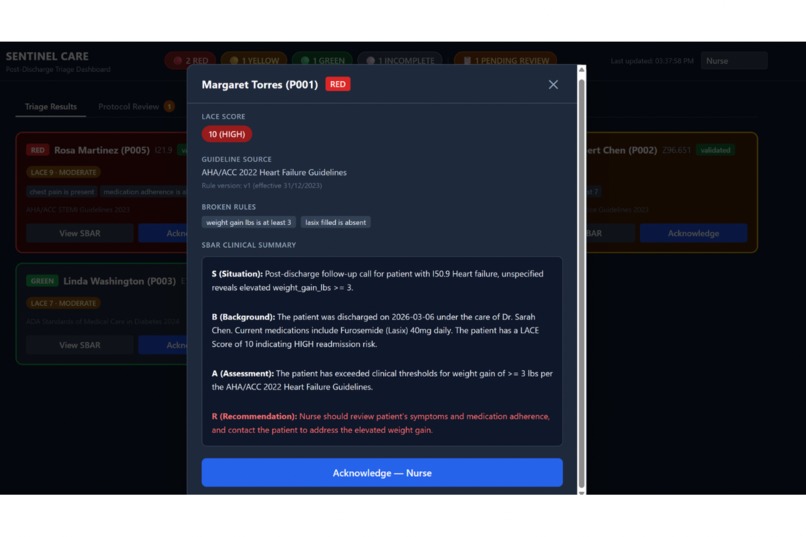
SBAR clinical summary modal for Robert Chen showing Nova Lite's S/B/A/R breakdown with nurse acknowledge button.
-
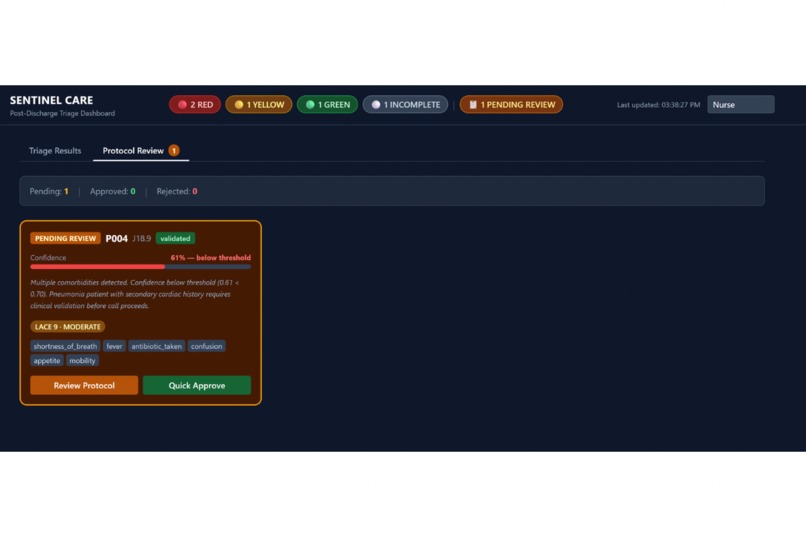
Protocol Review tab showing P004 flagged as PENDING with 61% confidence below threshold, awaiting nurse approval.
-
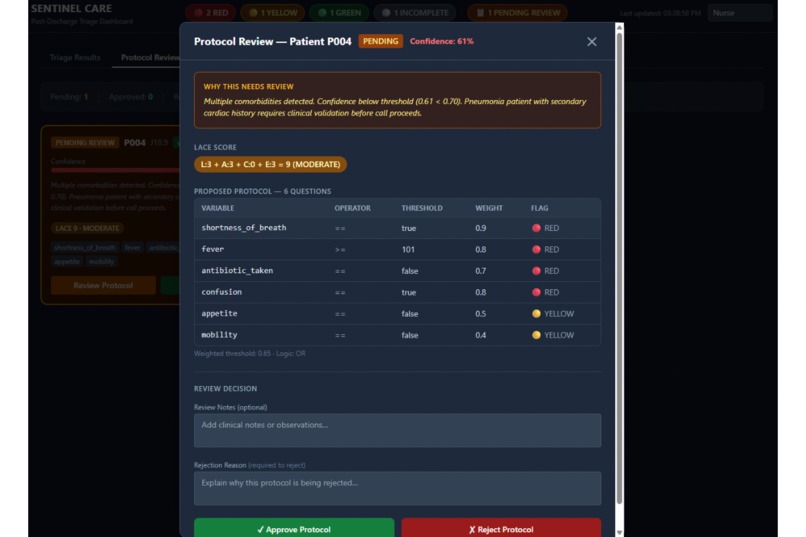
Protocol detail modal for P004 displaying Nova Pro's 6-question clinical protocol with RED/YELLOW flags and Approve/Reject buttons.
Inspiration
Sentinel Care was inspired by a real experience within our team. One of the team member, Kush, was involved in an accident and was later diagnosed with a herniated disc between L4 and L5. After discharge, we realized that recovery does not end when a patient leaves the hospital. In many cases, the most uncertain part begins at home, monitoring symptoms, following instructions, managing medications, and knowing when a change is serious enough to seek help. That experience made the post-discharge gap feel immediate and real to us.
It also made us think about a larger healthcare problem. Many patients leave the hospital with medications, discharge instructions, and recovery plans, but meaningful follow-up after discharge is still often manual, inconsistent, and difficult to scale. Traditional phone trees are frustrating, especially for older patients, and nurses can spend valuable time calling stable patients while urgent cases may be missed. We wanted post-discharge follow-up to feel like a continuation of care, not the end of it, so patients feel supported, monitored, and genuinely cared for after leaving the hospital.
That is why we built Sentinel Care: a voice-native post-discharge care platform that combines personalized outreach, structured clinical reasoning, and nurse-centered decision support. Instead of making patients feel like they were discharged and forgotten, we wanted to build something that makes follow-up feel timely, human, and clinically meaningful.
What it does
Sentinel Care is an Amazon Nova-powered post-discharge care platform that conducts personalized voice follow-up after a patient leaves the hospital. It asks clinically relevant questions based on the patient’s condition, detects warning signs from the conversation, and updates a real-time nurse dashboard with the patient’s triage status and structured summary. The goal is to help nurses identify which patients need urgent attention first while making follow-up more natural and more scalable.
The system uses three Amazon Nova models, each chosen for a specific reason. Nova Pro is used for care planning because it can reason over structured FHIR patient data and condition-specific clinical rules to generate a personalized triage protocol instead of a one-size-fits-all script. Nova 2 Sonic is used for the voice layer because Sentinel Care is built around natural, bidirectional voice interaction rather than a rigid phone tree. It uses FHIR context to personalize the call, including identifying the patient by name and asking condition-specific questions. Nova Lite is used for extraction and summarization because, after the conversation, the system needs to turn spoken responses into structured variables and concise nurse-facing summaries. In Sentinel Care, Nova Lite generates SBAR summaries, where SBAR stands for Situation, Background, Assessment, and Recommendation, a standard clinical format for communicating a patient’s condition and next steps clearly.
A key design principle in Sentinel Care is that AI does not make the final patient care decision. The system can produce a structured RED / YELLOW / GREEN recommendation through a deterministic TypeScript triage engine, but the nurse remains the final decision-maker for follow-up, escalation, and care action. That human-in-the-loop approach is central to the way we designed the system.
Another important design choice is how Sentinel Care handles patient responses. If a patient gives a long, unclear, or off-topic answer, the system can repeat the question to capture the specific response needed for rules-based triage. This is intentional, the system focuses on the clinically important signals required for evaluation, while richer call details can still be reviewed later by the nurse if needed.
How we built it
We built Sentinel Care as a TypeScript monorepo because the project includes many connected parts that need to stay consistent: shared schemas, validation, LACE scoring, clinical rule logic, multiple Lambda services, scripts, and a Next.js nurse dashboard. A monorepo let us reuse the same types and domain models across frontend and backend, reduce integration issues, keep validation logic centralized, and make the system easier to test and evolve as one platform rather than a set of disconnected services.
On the backend, we built modular services for care planning, answer extraction, SBAR summarization, outbound call initiation, answer collection, call completion, Nova Sonic handling, and a call bridge between Amazon Connect and the conversational voice layer. The frontend is a Next.js dashboard that supports real-time patient prioritization, SBAR viewing, acknowledgment workflows, and protocol review.
Our AWS stack includes Amazon Connect for outbound calling, AWS Lambda for service logic, DynamoDB for operational data, Amazon S3 for audio-related assets, Amazon SNS for escalation, Amazon Kinesis Video Streams for call streaming, AWS Step Functions for workflow orchestration, and an EC2-hosted HAPI FHIR server for structured patient data. We also built seeded demo patients, protocol review flows, rule versioning, and repeatable scripts so the full review → call → triage → SBAR journey can be demonstrated reliably.
Architecturally, we designed Sentinel Care around what we called a clinical AI sandwich: AI generates → deterministic engine evaluates → nurse decides → AI summarizes. Nova Pro creates the personalized protocol, the TypeScript triage engine evaluates answers against validated rules, the nurse remains in control of the final care decision, and Nova Lite generates the nurse-facing SBAR summary. This separation made the system safer, clearer, and easier to justify in a clinical workflow.
The live voice workflow works end to end. After a personalized call is completed, the system updates the patient’s latest triage result on the dashboard. If a newer call is made later, the older triage state is removed and replaced by the latest one, so nurses always see the most current assessment instead of outdated information.
Challenges we ran into
One of the biggest challenges was orchestrating a real-time voice workflow across multiple services. Sentinel Care had to connect Amazon Connect, Nova 2 Sonic, Lambda functions, DynamoDB state changes, FHIR-based patient context, and the dashboard into one end-to-end experience. Making the system personalized, stateful, and robust enough for a live demo required a lot of service coordination, test coverage, and fallback planning.
Another challenge was balancing natural conversation with structured clinical evaluation. We wanted the interaction to feel human and personalized, but our triage workflow still needed specific, rules-based answers. That meant building logic to handle long or unclear patient responses by repeating questions when needed, so the system captures only the clinically relevant information required for safe triage while preserving fuller details for later nurse review.
We also had to think carefully about guideline versioning, protocol approval, auditability, and demo reliability. Clinical rules are versioned, protocol review happens before calls are placed when validation is needed, and we built repeatable demo scripts so the full workflow can be shown consistently.
Accomplishments that we're proud of
We are proud that Sentinel Care is not just a concept or UI mockup, it is a full system with real architecture, real infrastructure, and a clear clinical workflow. We built a multi-model Amazon Nova pipeline where each model has a distinct responsibility, a deterministic triage engine for structured evaluation, and a real-time nurse dashboard that surfaces urgency and SBAR summaries in a way that is actionable.
We are especially proud that the voice AI works end to end as a real personalized follow-up experience. The system can use FHIR data to personalize the call, identify the patient by name, ask condition-specific questions, capture structured responses during the call, and update the latest triage result on the dashboard in real time.
We are also proud of the latest-state update design. Instead of stacking outdated results, Sentinel Care replaces the old triage state with the newest one after each completed call, which makes the dashboard more useful for real clinical follow-up.
We are also proud of the engineering depth behind the project. Sentinel Care includes shared schemas, FHIR-based LACE scoring, input validation, audit logging, rule versioning, protocol review workflows, a pure TypeScript evaluator, and deployed AWS resources across Lambda, DynamoDB, Connect, and EC2. The project also includes strong test coverage across schemas, validation, LACE logic, triage logic, extraction, and Nova Sonic simulation scenarios.
Most importantly, we are proud of the product vision behind Sentinel Care. We built something intended to make post-discharge follow-up feel more human for patients and more useful for nurses, something that extends the sense of care beyond the hospital rather than letting recovery feel disconnected after discharge.
What we learned
The biggest thing we learned is that useful healthcare AI is not just about using a powerful model. It is about assigning the right job to the right model, defining safety boundaries clearly, and designing a workflow that clinicians can actually trust. That is why Sentinel Care uses Nova Pro for personalized care planning, Nova 2 Sonic for natural voice interaction, and Nova Lite for extraction and SBAR summarization, while keeping the nurse as the final human decision-maker.
We also learned that in healthcare, natural conversation alone is not enough. A system may sound human, but it still needs to capture the right structured signals for safe decision support. That is why we built Sentinel Care to repeat questions when necessary, focus the triage engine on the most important answers, and still preserve fuller details for nurse review.
We also learned the value of building with a shared system architecture. The TypeScript monorepo approach made it much easier to keep schemas, triage logic, validation, and dashboard behavior aligned across the project. From an engineering perspective, we learned a great deal about AWS voice orchestration, FHIR-based patient modeling, deterministic clinical logic, real-time dashboard workflows, and how to turn a technically complex system into a clear hackathon product.
Overall, we learned that the strongest healthcare products are not the ones that try to replace nurses, they are the ones that help nurses focus faster, act with better context, and maintain trust with patients during vulnerable transitions of care.
What's next for Sentinel Care
Our next step is to evolve Sentinel Care from a hackathon prototype into a production-ready care coordination platform. That includes stronger authentication, more robust deployment isolation, broader condition coverage, richer escalation workflows, and tighter integration with clinical systems.
A major priority for the next phase is HIPAA-compliant deployment and data handling. That means moving toward secure healthcare-grade infrastructure with stronger access control, encryption for data in transit and at rest, audit logging, role-based permissions, secure storage of patient information, and architecture choices aligned with HIPAA requirements for protecting sensitive health data.
We also want to strengthen the clinical workflow by expanding nurse review controls, improving protocol approval and escalation paths, and supporting better monitoring over time instead of only a single follow-up interaction. A future improvement we want to add is a callback workflow. If a patient misses the call, disconnects early, or the interaction is incomplete, the system should be able to automatically place a callback or offer a reconnect option so the follow-up can be completed reliably.
In the long term, we see Sentinel Care growing into a broader voice-native post-discharge intelligence platform that helps hospitals stay meaningfully connected to patients after discharge while keeping nurses in control of final care decisions.
Built With
- amazon-connect
- amazon-ec2
- amazon-kinesis-video-streams
- amazon-lex
- amazon-nova-2-sonic
- amazon-nova-lite
- amazon-nova-pro
- amazon-sns
- amazon-web-services
- aws-lambda
- aws-step-functions
- dynamodb
- hapi-fhir
- next.js
- npm
- react
- typescript
- zod




Log in or sign up for Devpost to join the conversation.