-
-
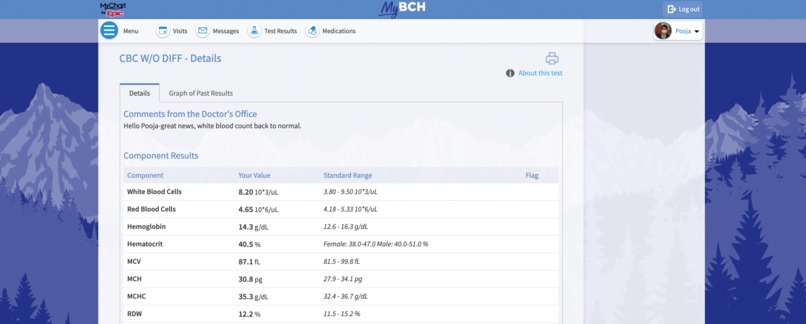
Example EHR Integration
-
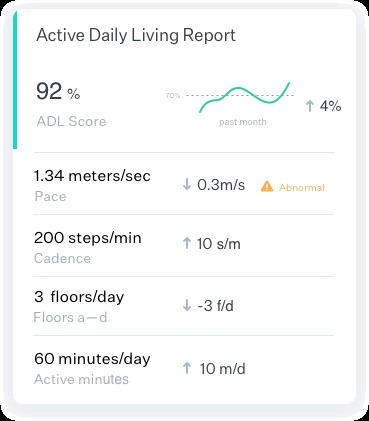
Example Active Daily Living Report Module/Embed
-
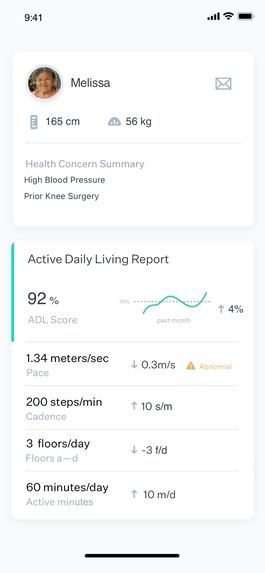
Example Active Daily Living Report iPhone Screen
-
Example Notification
-
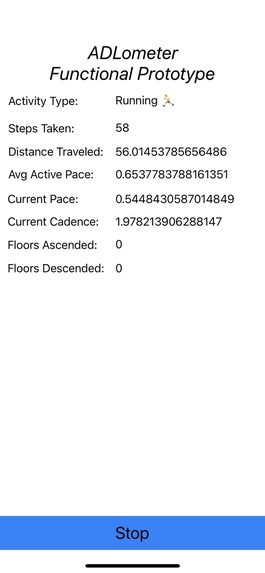
Functional Prototype Screen Correctly Identifying Activity Type (Running) and Capturing Key Metrics
-
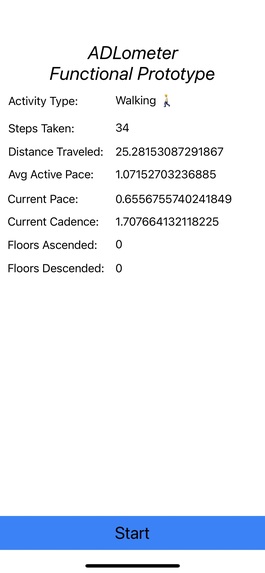
Functional Prototype Screen Correctly Identifying Activity Type (Walking) and Capturing Key Metrics
-
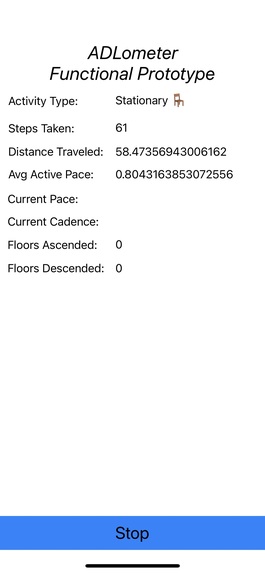
Functional Prototype Screen Correctly Identifying Activity Type (Stationary) and Capturing Key Metrics
Inspiration
Activities of daily living (ADL) are defined as essential and routine tasks that can be performed by healthy individuals without assistance. Unfortunately, as an individual ages, their ability to perform these tasks starts to wane, leading to unsafe conditions and a poor quality of life.
This reduction is insidious – patients do not notice a decrease in their ability until much later in their pathophysiological process. The ability to accurately, constantly, and non-invasively assess one’s ADL status remains one of the biggest challenges in Geriatrics. If patients themselves are not consciously aware of their deficiencies, they are unable to communicate them to their caregivers and medical team. Consequently, the patients forego more effective preventative treatments.
Additionally, individuals who spend continued time in a wheelchair or bed are at increased risk for pressure ulcers. Each year, more than 2.5 million people in the United States alone develop this skin degeneration, which brings not only pain but also increased risk for serious infection and increased health care utilization and even mortality. Current methods treat wounds after they occur, which misses an opportunity for prevention or monitoring for faster healing and a dramatic reduction in treatment cost. With the rise of COVID and the need to ration medical services effectively, a clear need exists for pressure ulcer prevention especially for people with reduced ADL scores.
What it does
I built an iPhone application that can classify activity type (running, walking, driving, cycling, and stationary) using a wide range of input sources such as the accelerometer, gyroscope, magnetometer, and pedometer. These metrics are then combined to generate an “Active Daily Living” report with an associated ADL metric, average daily pace, average daily cadence, average floors ascended/descended, and daily active minutes. The ADL metric will use a weighted combination of running, walking, driving, cycling, and stationary to develop an active-stationary percentage. For example, stationary and driving would yield activity weights of 1, whereas running would yield weights of 1.5. These metrics need to be fine-tuned and will be discussed in the Future Directions.
While this report does not completely capture the complexity of Basic and Instrumental ADLs (Eating, grooming, toileting, financial management), we hope that this report can serve as a useful screening tool with a high sensitivity to detect the most at-risk individuals for proper medical triage. This information is then safely and securely transmitted to the hospital EHR system using the secure Google Healthcare API.
Additionally, I also independently developed a neural network machine learning model that can classify activities as either walking or running based on only gyroscope and accelerometer sensor data. This serves as a proof-of-concept model to develop inexpensive, disposable bands that can integrate readily available sensors to classify activity and generate ADL reports in resource-limited settings and highly disposable settings (i.e., each patient in a hospital ward can have this technology integrated with their hospital ID wristband to prevent hospital bed-induced pressure ulcers).
Lastly, I was able to use this app to constantly track a patient’s stationary activity and develop an alerting system to prevent pressure ulcers. In short, if the patient is bedridden, in a wheelchair, or otherwise has a low ADL score, the application will remind the patient to shift their weight after a continuous inactivity period of 30 minutes. Additionally, if the individual does not have adequate upper body strength to perform this maneuver, the application will automatically contact the caregiver using the Twilio Text Messaging API.
Development Tools
I built this application using a combination of Python and Swift in Jupyter Notebooks and XCode, respectively. The project code is all available on our GitHub page.
Impact
My hypothesis is that through early detection of pressure ulcers we can create a significant reduction in the severity of pressure ulcers and consequent patient infection and mortality.
In addition, I believe there will be strong benefits to earlier detection of decreasing ADL, which allows for earlier healthcare (family, caregiver, or medical staff) intervention checkpoints. This system can result in the prevention of many of the significant mobility and health related challenges faced by the elderly.
What's next for ADLometer
Future directions for ADLometer include:
(1) Getting more data points to fine tuning the weights of the activity parameters instead of relying on user gestalt.
(2) This data would benefit from further integration with other continuous monitoring devices. In fact, I would like to reach out to existing wound care platforms like Dr. Yazdi’s Tissue Analytics to see if we can integrate this technology into their service.
(3) Further explore the possibility of creating inexpensive, disposable hospital wristbands that integrate cheaply, readily available gyroscope and accelerometer sensors to classify activity and measure ADL-related metrics.







Log in or sign up for Devpost to join the conversation.